ALOPECIA
Alopecia is the medical term for hair loss and is common in both men and women. Alopecia usually, and most noticeably, affects the scalp but can affect any part of the body where hair grows. Alopecia has many different causes and depending on the cause, different treatment will be recommended.
Normally hairs grow out of hair follicles in a cycle – the amount of time the hair stays in the ‘active’ part of the cycle determines the length of hair growth. As part of this cycle, it is normal to lose up to 100 scalp hairs per day as new hairs push the old hairs out of the follicle. If higher numbers of hairs are lost than is replaced, hair thinning or loss is seen.
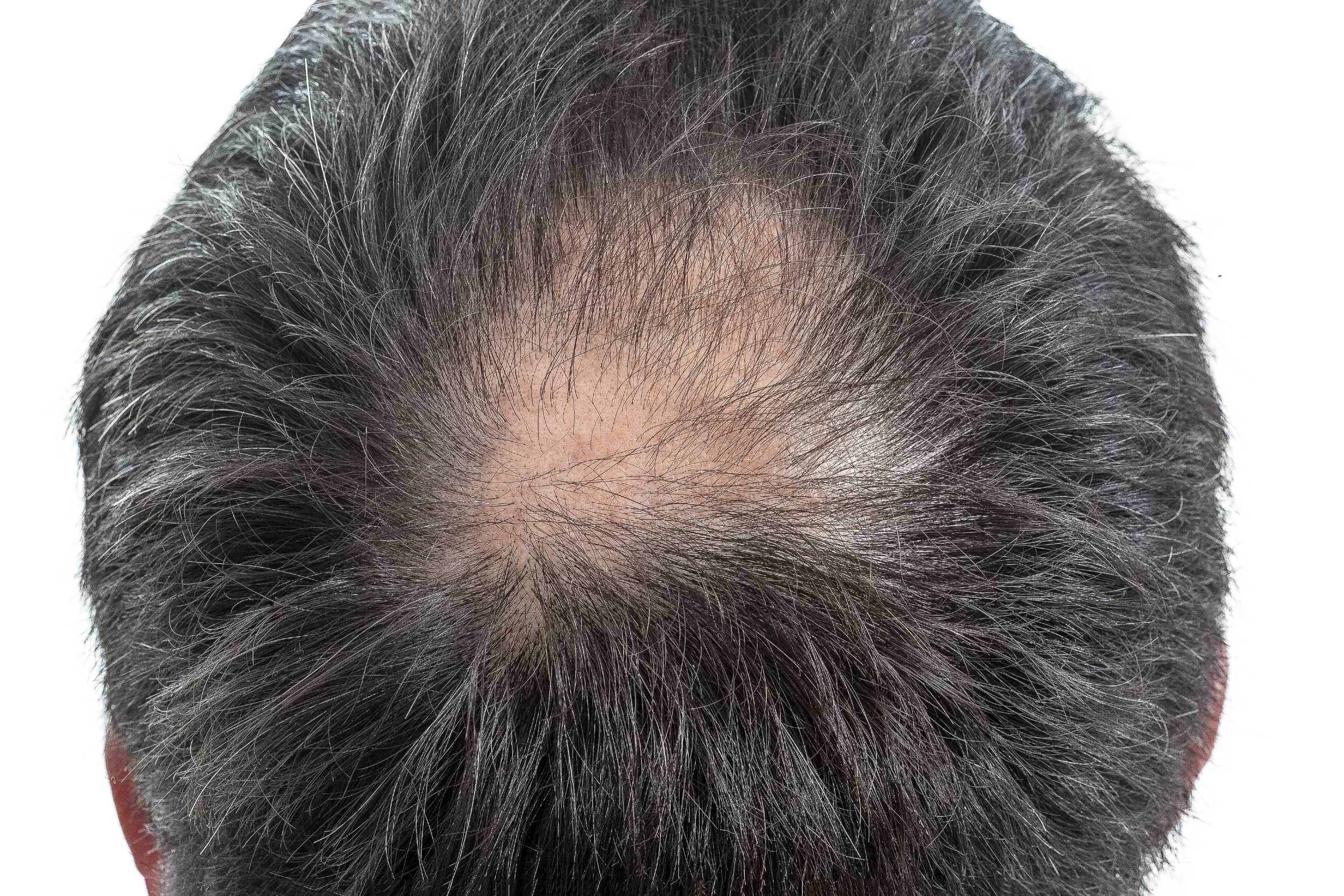
Types of hair loss include non-scarring alopecia, where the hair follicles are intact with the potential for hair to re-grow and scarring alopecia, where the hair follicles are destroyed so that hairs cannot grow back. Below are the most common causes of alopecia, grouped in to these main types.
